The importance of equipment localisation assigned to Covid cases

Introduction
In some hospitals, a sorting between patients is already being discussed, favouring Covid patients at the expense of the other possible cases of hospitalisation. This can lead to rescheduling of surgeries (for some that have been planned for a long time but that are not vital) in order to face the shortage of materials in the ICU. But all these decisions will not stay without consequences on the health and comfort of the patients. It is essential to find solutions to help the medical staff in their handling of the crisis.

Real-Time location system in hospitals: A solution for equipment shortages and patient care
During the first wave, the congestion relief in urban hospitals was done by sending patients to less congested hospitals in the countryside. Today, geolocation can provide a less radical solution : by using Bluetooth Low Energy (BLE) radio waves, a real time location system (RTLS) can locate all types of equipment tagged with a precision of 2-3 meters. This system is takes the form of waterproof and robust IoT devices, which can be easily fixed on equipment. In hospitals, this type of geolocation system can also be used to locate beds, respirators and any other material actually needed to treat coronavirus patients, helping the medical staff by using the web and mobile app to have a quick overview of the equipments’ location in all units in real time.

By localising all the equipment in the building, a great amount of time is saved and the medical staff can also evaluate their availability: the equipment located in a storage place will be marked as available whereas the others, located in patient’ rooms, will be marked as being in use. It will be the same for beds and stretchers, the most affected by the lack of availability despite the increase of their numbers in the ICU since the beginning of the crisis. With the inventory in real time, the hospitals can more easily anticipate treatment of new Covid cases by determining how many patients can be taken care of in the units and especially in the ICU, where the influx is the most important. This way, patient care will be improved thanks to reduced waiting time which was often caused by medical staff’s time spent on checking equipment’ availability in the units.

Medical staff, who are exhausted and demoralised by this unprecedented sanitary crisis, will see their morale improve. Geolocation could bring practical assistance and therefore release. No need for staff to run everywhere to find an artificial respirator for a patient in respiratory distress, when they can simply see on a smartphone where the closest available respirator is. To count available equipment quickly, an option exists to calculate the number of equipment with a tag in a zone defined by the user which can go from one room to the entire hospital. Having this information on-hand makes it much easier to know the availability of equipment quickly. The time saved can be allocated back to time spent for the patients’ care. Thanks to this system, there will be less weight and stress on the medical staff.

Using RTLS to anticipate capacity and avoid saturation in hospitals
To conclude, geolocation can help improve coordination between hospitals of the public and private sectors. By closely monitoring equipment availability, it gives them the ability to anticipate the capacity each hospital has to receive new infected patients. Thus, when a healthcare facility sees that it has insufficient resources compared to the influx of patients, it will have the possibility to contact the surrounding facilities in order to allow a redirection of patients to the less overloaded hospitals and private clinics. It will be the same for a patient in the ICU: when a new case will be declared and no oxygen equipment is available, it will be possible to transfer the patients to another hospital who has the necessary equipment. Saturation of critical care capacity could therefore be avoided.
The geolocation can therefore bring strong value to hospitals by helping them manage better operations and provide better patient care for the comfort of both patients and medical staff.
The geolocation is a real advantage for the hospitals, by providing a help in the operational management of the sanitary crisis, and by improving the comfort of the patients and medical staff.
News that might interest you

BLE ESL and RTLS Integration in Manufacturing
Ubudu’s BLE ESL integration with its RTLS delivers real-time asset tracking and automated updates for manufacturing. Featuring dynamic ESL displays from brands like PDI Digital and Minew—with options in size, interchangeable batteries, and shock protection—this solution streamlines workflows using a wireless BLE network, available via SaaS or on-premise.

The power of Hybrid RTLS solutions
Hybrid RTLS combines the benefits of different location tracking technologies to provide the most efficient results for tracking needs and can be used for multiple use cases. As indoor and outdoor positioning become increasingly interconnected, it is important to consider how to combine different RTLS technologies to improve ROI and meet the needs of end-users.
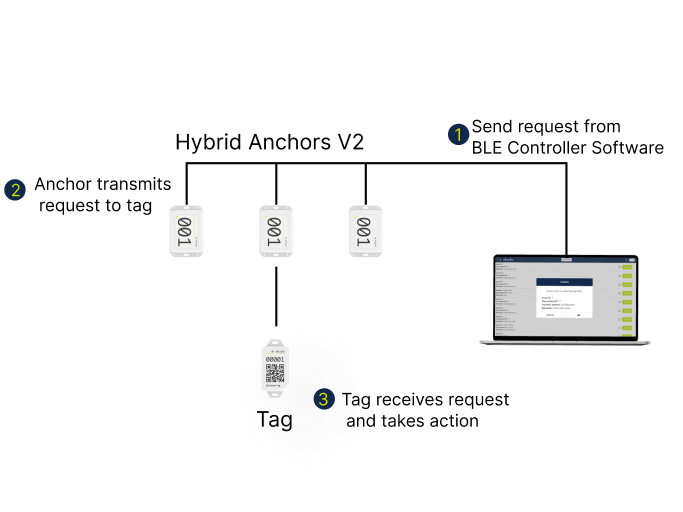
Introduction to Ubudu BLE Controller
Ubudu launches “BLE Controller”, a new feature available in Ubudu RTLS that will enable you to communicate with any RTLS tag remotely, right from your desk.




